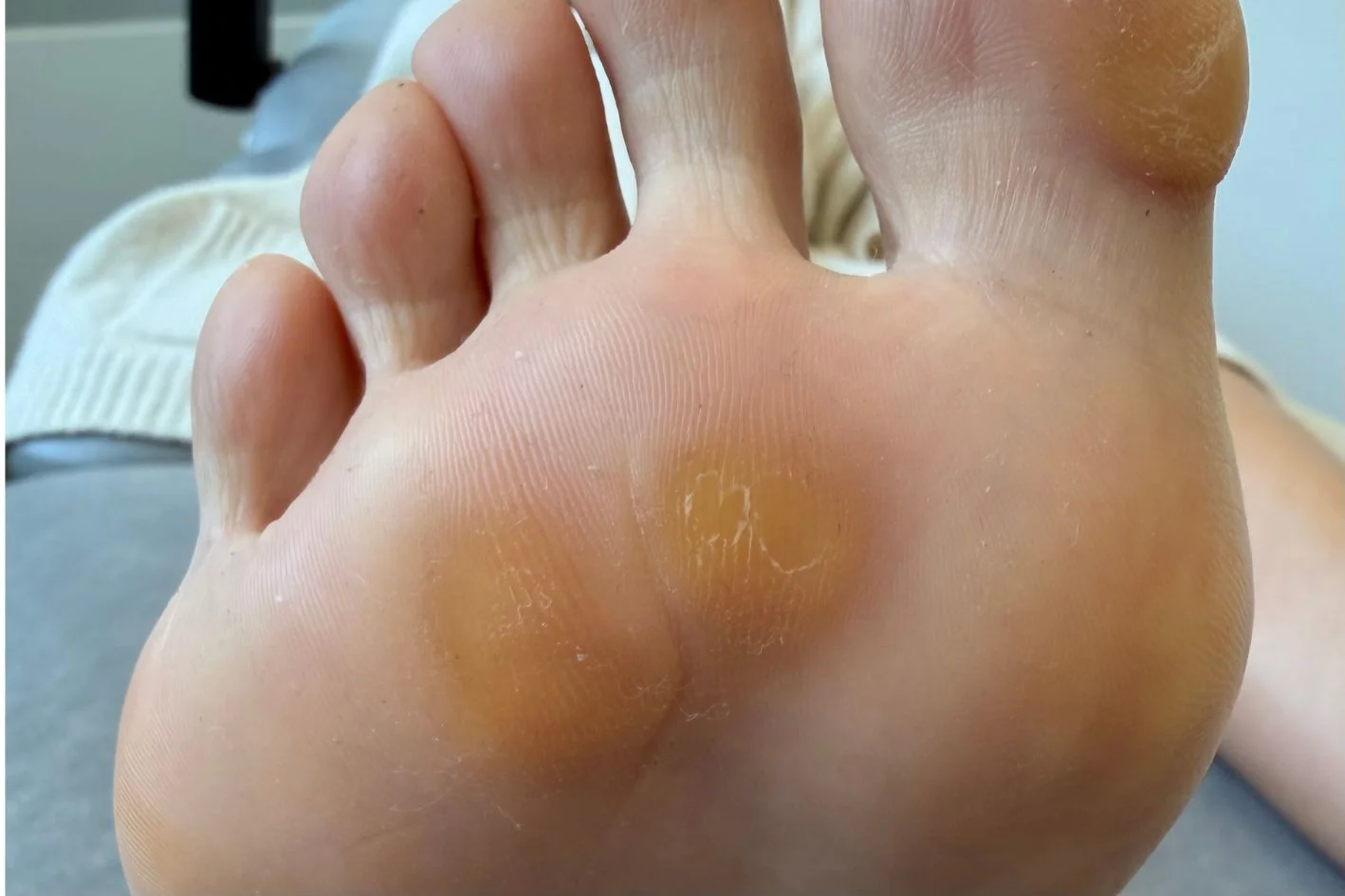
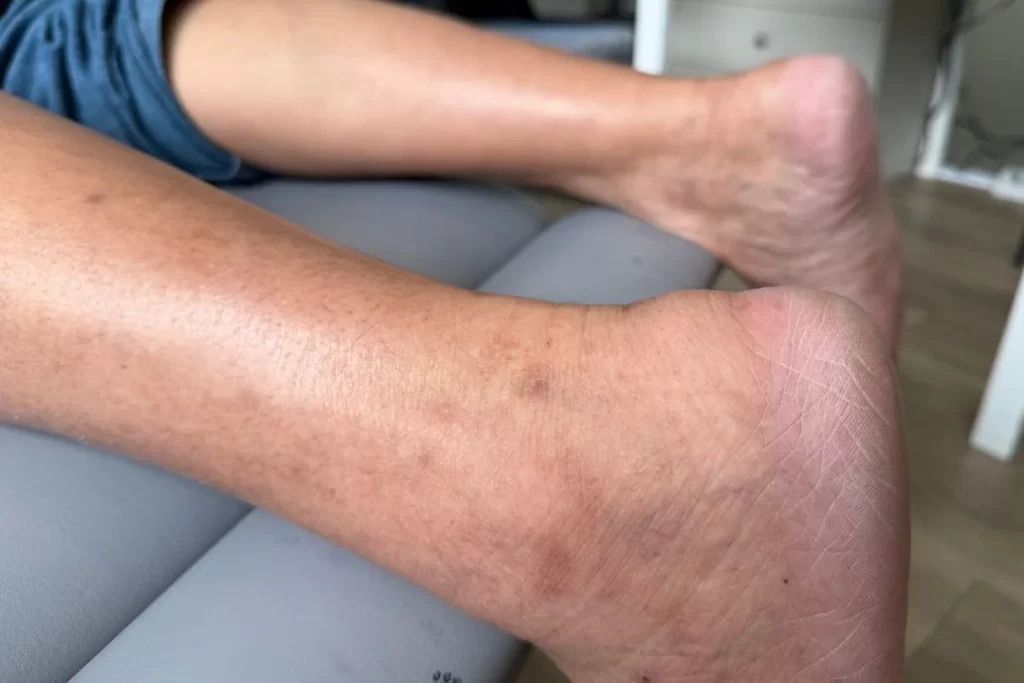
Have you noticed patches of skin on your feet becoming thicker, rougher, or harder than the surrounding area, particularly beneath the toes, across the balls of your feet, or around the heels? These areas might be foot calluses, which develop as a protective response to repeated friction or pressure. Although a callus on the foot might be painless early on, it can start to feel uncomfortable when the hardened area builds up or keeps returning.
Skin doesn’t usually thicken for no reason. In most cases, calluses on feet develop when certain areas are exposed to repeated stress during standing, walking, or daily activity. This might be linked to footwear, foot shape, gait patterns, or recurring load on the same part of the foot. Over time, what begins as a small rough patch can become more noticeable, more compact, and harder to ignore.
Understanding foot callus causes is useful because removal alone doesn’t explain why the skin keeps building up in the same spot. To manage a foot callus properly, it helps to recognise how it presents, where it tends to form, and when it might start causing discomfort, which is why it makes sense to begin with the symptoms.
Symptoms of Foot Calluses
A foot callus might not seem especially troublesome at first, which is why it’s often ignored in the early stages. However, when pressure or friction continues in the same area, the signs can become easier to notice and, in some cases, harder to ignore.
- Thickened, rough, or hardened patches of skin.
- Dry skin with a yellowish or greyish appearance.
- Reduced sensitivity over the affected area.
- Callus build up beneath the toes, across the ball of the foot, or around the heel.
- Tenderness or discomfort during walking or standing.
- Pain as the thickened skin becomes more pronounced.
- Cracks or fissures within the hardened skin, especially around the heel.
- Greater risk of irritation or infection when deeper splits are left untreated.
Once a foot callus begins to develop, the changes aren’t always limited to appearance alone. In some cases, it remains a minor skin issue for a period of time, but when pressure continues to build in the same area, it might start to affect comfort as well. This is often the point where people begin to notice that the problem is becoming more persistent rather than simply superficial.
While calluses are often asymptomatic in their early stages, persistent pressure or friction can irritate them over time, leading to tenderness or discomfort during activities like walking or standing. As they grow thicker, these hardened areas can become painful. In more severe cases, cracks or fissures may form within the callus, causing significant pain and increasing the risk of infection if left untreated.
Need Help? See A Podiatrist Today
Types of Foot Calluses
Foot calluses can develop in different ways. Their shape, location, and structure often reflect the kind of pressure or friction affecting the foot over time, which is why one foot callus might remain relatively mild while another becomes more painful or persistent. Recognising these patterns is useful because it helps show what’s causing the build-up and what sort of care is needed for pain relief and to help prevent recurrence.
Pinch Calluses
Pinch calluses develop when the skin is repeatedly compressed or squeezed, usually by tight footwear. They’re often found on the little toe or along the edge of the big toe, where pressure is concentrated within a small, localised area.
Plantar Calluses
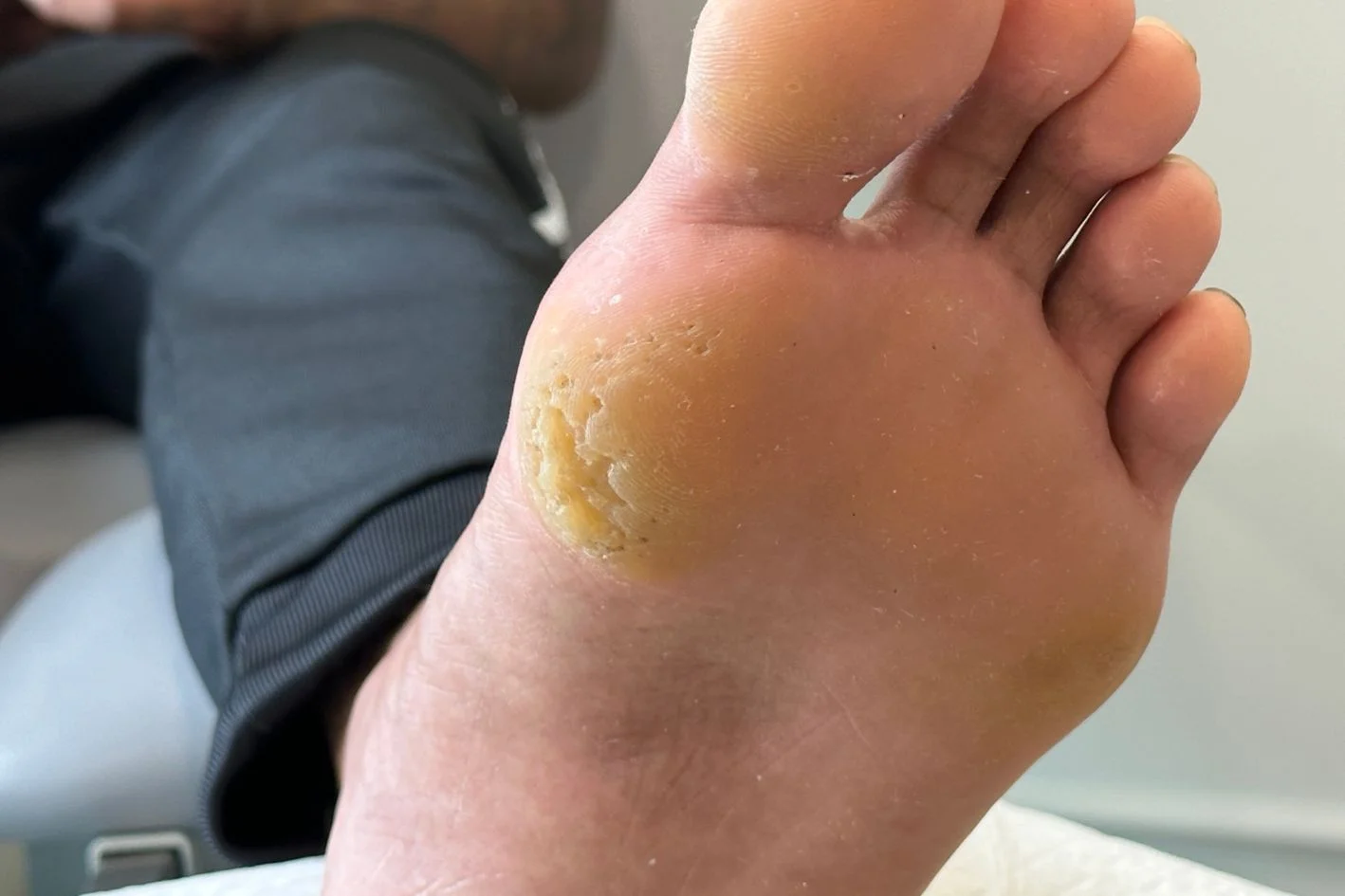
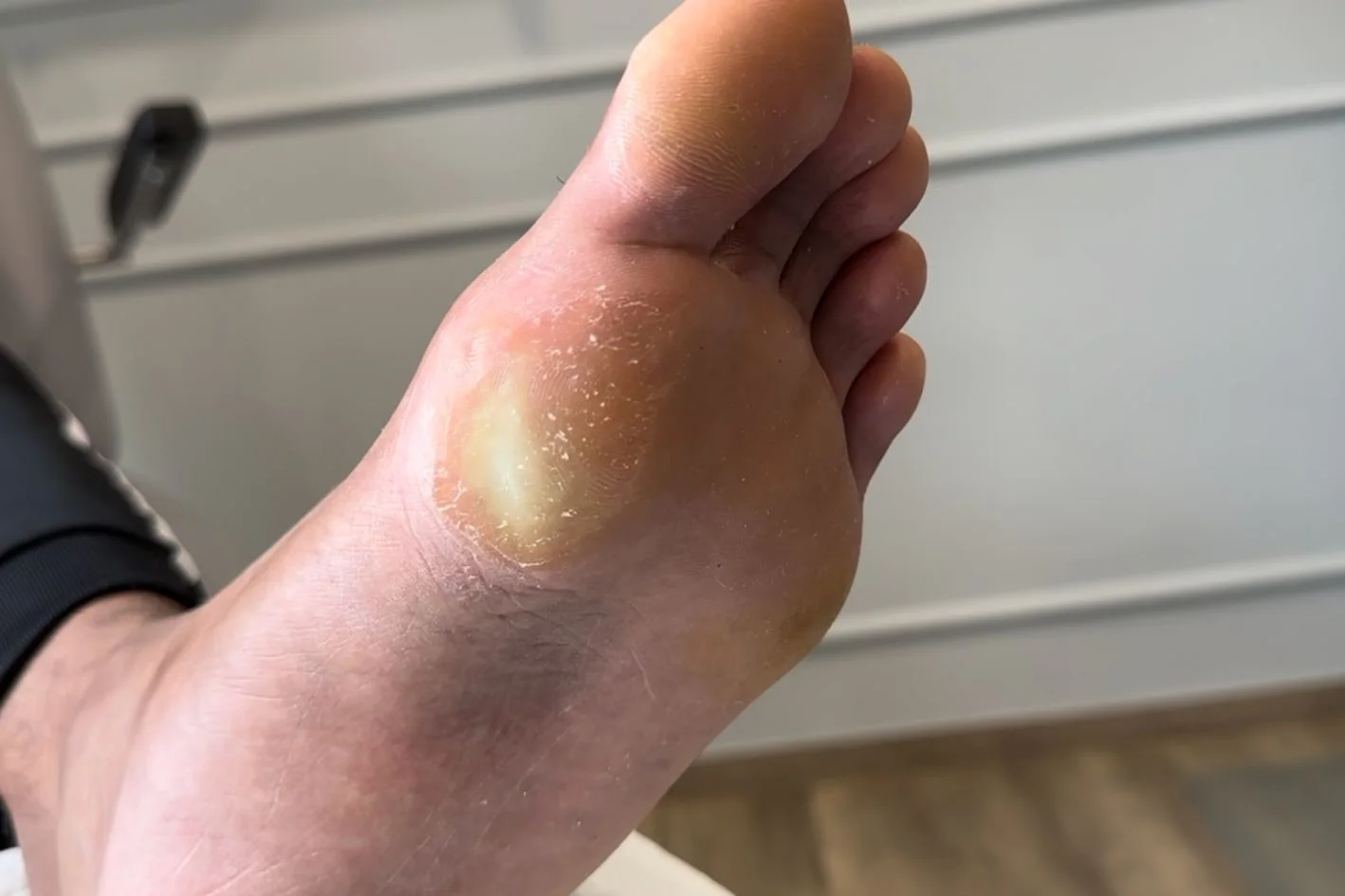
Plantar calluses develop on weight bearing areas beneath the forefoot, especially under the ball of the foot. These are the most common type of foot callus and usually appear where repeated loading causes the skin to become broader, flatter, and harder over time.
Heel Calluses
Heel calluses develop around the rim of the heel, where repeated loading causes the skin to harden and dry out over time. When the thickened skin becomes less supple, it can split and lead to cracked heels (fissures).
Structural Subtypes of Foot Calluses
Foot calluses can also differ in their internal structure, not just their location. These subtypes help explain why one lesion stays broad and superficial while another becomes more localised, more painful, or more difficult to manage.
- Discrete nucleated callus – This is a localised and often painful callus with a dense central keratin plug that presses into the tissue beneath. Because of its appearance, it can sometimes be mistaken for a plantar wart, although it’s not caused by a virus.
- Diffuse shearing callus – This is a broader area of thickened skin that usually measures more than one centimetre across and doesn’t contain a central keratin plug. Instead, it spreads across the surface in response to repeated shear and load.
- Plugged callus – This is an inward-growing callus with a dense hardened core that presses into the foot rather than building outward. This inward pattern can cause significant discomfort, especially during walking, standing, or other prolonged activity.
Stages of Foot Calluses
As foot calluses continue to build up, the skin can undergo different stages of thickening and structural change. Over time, this can affect not only how the area looks, but also how it feels during walking, standing, and other daily activity.
- Stage 1 – The callus is only lightly thickened and appears as a thin layer of hardened skin. At this stage, the area might feel slightly rough or dry, but it usually remains painless and relatively supple.
- Stage 2 – The callus becomes more noticeable, with greater thickening and a firmer texture. As pressure continues, discomfort can begin to develop during walking, standing, or other repeated activity.
- Stage 3 – The callus shows clearer structural change, with concentric keratin plugs developing within the thickened skin. These denser areas can cause more localised pain, especially when direct pressure is applied.
- Stage 4 – The callus becomes more advanced, with deeper hardening and more pronounced density change within the skin. At this stage, fissures or cracks might form, leading to pain and a higher risk of infection.
Causes of Foot Calluses
A foot callus usually develops because one area of skin keeps dealing with more stress than it can comfortably tolerate. This often happens when external factors such as footwear or activity combine with underlying factors such as foot shape, skin quality, or gait. Looking at these causes more closely helps explain why some calluses keep returning to the same part of the foot.
What Increases Friction or Pressure on the Foot?
- Footwear that is tight, loose, poorly cushioned, or high heeled can increase pressure and rubbing across different parts of the foot.
- Shoes that allow the foot to slide repeatedly can keep stressing the same weight bearing areas over time.
- Going without socks, or wearing socks that don’t fit properly, can increase friction during daily activity.
- Standing, walking, sports, work, or other repetitive activity can keep loading the same parts of the foot and encourage thicker skin to develop.
Who Carries Higher Baseline Risk?
- Inherited foot shape or structure can make some people more prone to repeated pressure in certain parts of the foot.
- Certain walking patterns or foot mechanics can keep shifting load onto the same area over time.
- Skin that is naturally drier or less resilient can be more prone to thickening under repeated stress.
- Ageing, skin conditions such as psoriasis or eczema, and factors that contribute to dryness can also make callus build up more likely.
Note: People with diabetes should pay closer attention to foot calluses, as reduced sensation can make thickened skin harder to notice. If the area cracks or breaks down, this can increase the risk of ulceration and infection.
Conditions Commonly Mistaken for Foot Calluses
Not every thickened or painful patch of skin on the foot is a callus. Some conditions can look similar at first because they also cause local discomfort or skin changes in weight bearing parts of the foot. This is why it’s important to identify the exact cause, since management can differ depending on what is actually affecting the foot.
- Foot corns – These also develop from repeated pressure or friction, but they are usually smaller, more localised, and more likely to have a firm central core. By contrast, foot calluses are often broader, flatter, and spread across a wider area of skin.
- Plantar warts – These can also be mistaken for foot calluses, especially when a callus is more localised or has a dense central keratin plug. Unlike calluses, plantar warts are caused by a virus and might interrupt the natural skin lines or show small black dots.
Managing and Preventing Foot Calluses
Foot calluses can persist when the same area of skin is exposed to repeated friction or pressure on a regular basis. Because of this, management isn’t just about reducing the thickened skin itself, but also about addressing the factors that caused it to build up in the first place. At the same time, the approach can vary depending on where the foot callus is located, how thick it has become, whether it’s causing pain, and whether dryness or cracking are also part of the problem.
To start, the focus is on reducing irritation and limiting further stress through the affected area while keeping daily activity more comfortable:
- Avoid cutting, picking, or digging at the callus yourself, as this can worsen irritation and damage the surrounding skin.
- Choose footwear that fits well, with enough room and cushioning to reduce rubbing and pressure across the foot.
- Wear socks that fit properly and help reduce friction during walking, standing, and other daily activity.
- Use protective padding or heel cups where appropriate to reduce repeated pressure on the affected foot area.
- Gently use a pumice stone or foot file to manage dead skin build up, ideally when the skin has softened after bathing or soaking.
- Apply moisturiser regularly to help keep the skin softer and reduce excessive hardening, especially around the heel.
When a foot callus becomes painful, keeps returning, or is linked to an underlying pressure problem, podiatry care can help address it more directly:
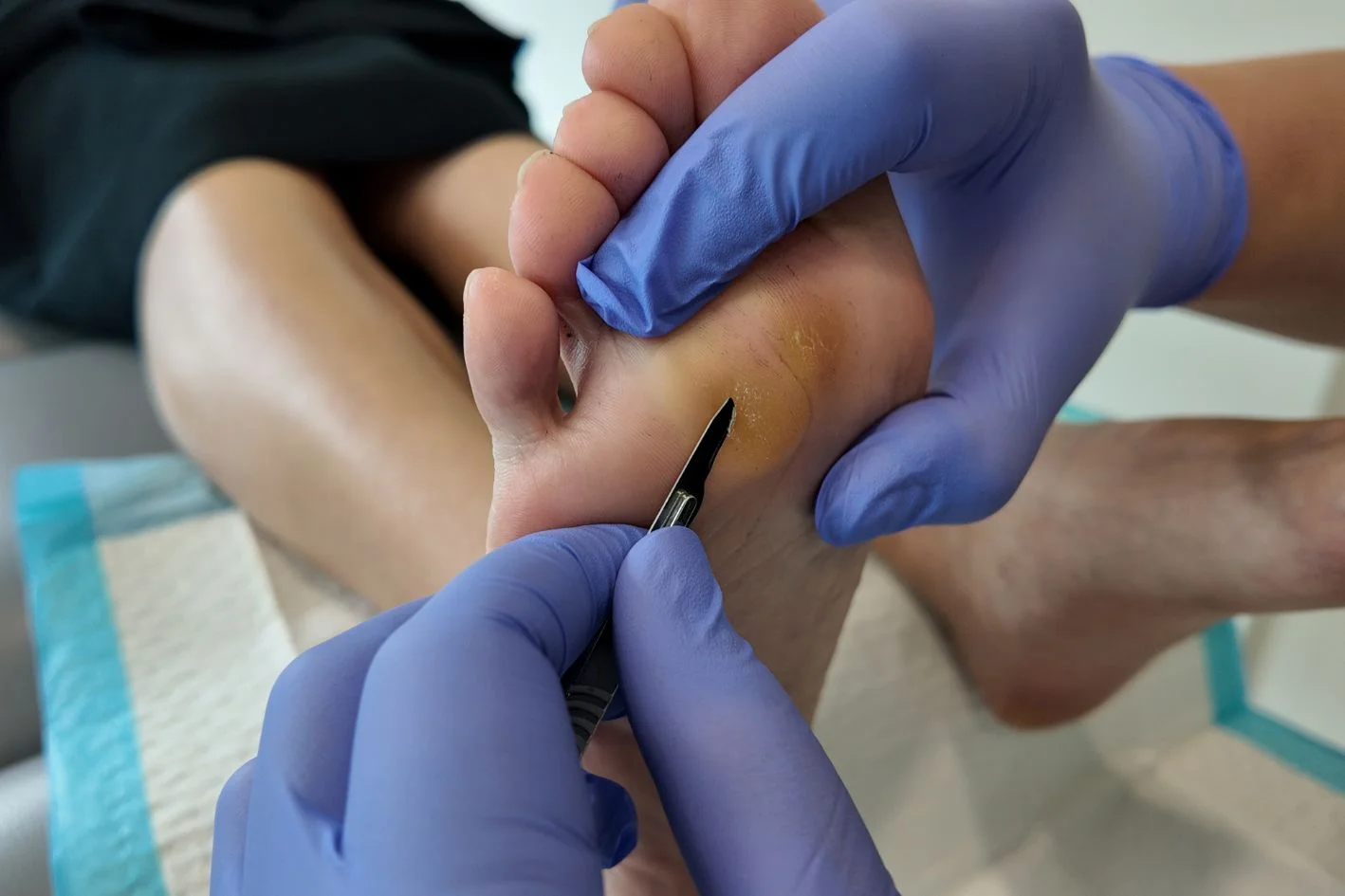
- Debridement can reduce thickened skin carefully, helping relieve pressure and improve comfort during walking and shoe wear.
- Footwear advice can help when poor shoe fit, limited cushioning, or repeated rubbing is contributing to the problem.
- Pressure assessment can help identify whether foot shape, posture, or gait pattern is driving repeated stress through one area.
- Custom orthotics might be recommended when more tailored support is needed to redistribute pressure away from the affected area.
- Structural problems such as bunions, hammertoes, or altered foot mechanics might also need attention when they are contributing to repeated pressure.
If a foot callus remains painful and continues to affect walking comfort or footwear choice, assessment by a podiatrist can help clarify what’s placing repeated stress on that area. This allows management to be directed not just at the foot callus itself, but also at the underlying factor contributing to it. People with diabetes or poor circulation should also seek professional care earlier, as thickened skin can be harder to monitor and more prone to complications once cracking or breakdown begins.
Have Your Foot Callus Removed at Straits Podiatry
When a foot callus becomes painful enough to affect walking comfort or make certain shoes harder to wear, more targeted care is often needed. At Straits Podiatry, we assess whether the problem is truly a foot callus, identify the type involved, and look closely at the pressure, friction, or structural factor that is keeping that area under stress.
Once that’s established, we can then plan for the removal of it and management around what your foot actually needs. This might include careful debridement, footwear advice, padding or pressure relief measures, as well as more targeted podiatry care for cracked heel calluses or more complex foot callus subtypes. Speak with our team or book a consultation for an assessment and a personalised plan for the removal of your foot callus.
Frequently Asked Questions About Foot Calluses
What is a foot callus?
A foot callus is a patch of thickened, hardened skin that develops when one part of the foot is exposed to repeated pressure or friction over time. It commonly forms on weight bearing areas such as the sole, ball of the foot, or heel, where the skin responds by building up for protection. Although a callus is often dry, rough, and less sensitive than the surrounding skin, it can still become uncomfortable when the thickened area grows more pronounced or keeps returning.
How do I get rid of calluses on my feet?
Getting rid of foot calluses usually starts with softening and reducing the thickened skin while also lowering the pressure that caused it to form. This would include soaking the feet in warm water, gently using a pumice stone or foot file, and applying moisturiser regularly to keep the skin softer and less prone to hardening. However, if the callus persists, becomes painful, or keeps building up in the same area, podiatry care might be needed for professional debridement and advice on how to reduce recurrence.
Are foot calluses the same as foot corns?
Foot calluses and foot corns are related, but they aren’t the same. Both develop because of repeated pressure or friction, yet a foot callus is usually broader, flatter, and spread across a wider area of skin, especially on weight bearing parts of the foot. A foot corn, by contrast, is typically smaller, more localised, and more likely to have a firm central core, which is why it can feel sharper or more painful in a concentrated spot.
What is debridement of a foot callus?
Debridement of a foot callus is the careful removal of thickened, hardened skin that has built up from repeated pressure or friction. It’s usually performed by a podiatrist using appropriate instruments to reduce the callus without damaging the surrounding skin. This can help relieve discomfort, improve comfort during walking or shoe wear, and reduce the risk of cracking when the callus has become more advanced.
Do custom orthotics help with foot calluses?
Custom orthotics can help with foot calluses when repeated pressure keeps building up in the same part of the foot. By redistributing load more evenly, they can reduce strain on pressure points and help make recurrence less likely. If foot shape, gait pattern, or underlying mechanics are contributing to the problem, a podiatrist can advise on suitability and, if needed, make a pair tailored to your feet.
Share this with someone you know