Fungal Foot Symptoms, Causes, and Management
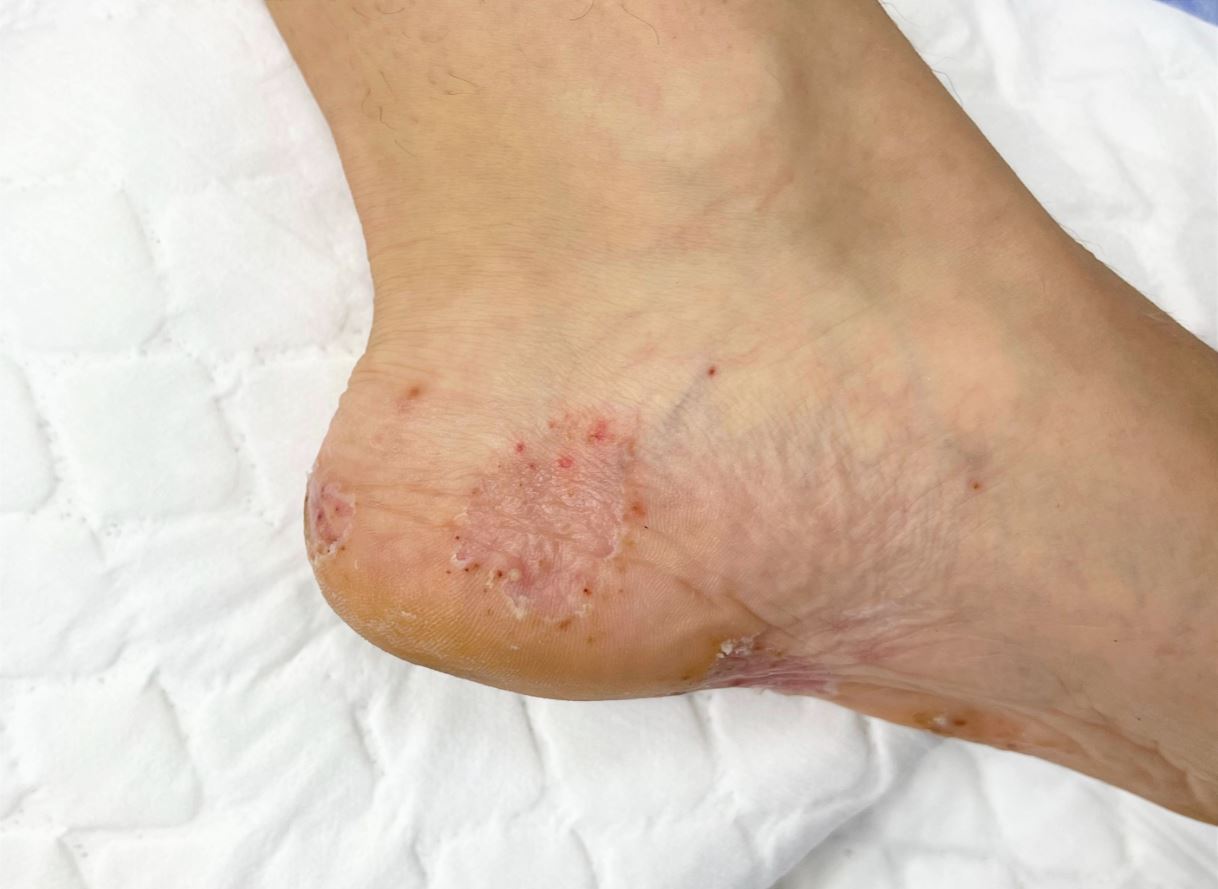
It often begins with an itch that’s hard to leave alone. At first, it might seem like a minor irritation between the toes. Yet the discomfort keeps drawing your attention back to the area, until scratching starts to make the skin feel even more irritated than before. As this continues, the skin might begin to peel, scale, soften from excess moisture, or crack between the toes. In more irritated cases, it can also become weepy or start to crust.
As these changes become more noticeable, fungal foot is one possible explanation. This is a fungal infection affecting the skin on the feet, and it often starts between the toes because that area tends to stay warm and moist more easily, especially when the feet become sweaty, stay enclosed in covered footwear for long periods, or remain damp after rain, wet shoes, or other prolonged exposure to moisture. This also helps explain why the infection is harder to clear once the skin stays wet for too long.
This condition is known medically as tinea pedis, though it’s more commonly known as athlete’s foot. In Singapore, some people also call it foot rot, an informal term used colloquially for this kind of fungal infection between the toes. Recognising it early matters, because once the signs are identified for what they are, the right steps can be taken to manage the infection and prevent it from worsening.
Symptoms of Fungal Foot
Fungal foot can show up in a few different ways, and not everyone will notice the same pattern. In many cases, it affects the skin between the toes first, although it can also involve the sole, sides of the foot, or heel. It might affect one foot or both, depending on how established the infection is.
- Itchy skin – Itching is often one of the earliest and most noticeable symptoms, especially between the toes, and might feel more obvious once footwear is removed.
- Peeling, scaling, or split skin – The skin might begin to peel, scale, or split, particularly between the toes where moisture tends to collect more easily.
- Softened or soggy skin – In some cases, excess moisture causes the skin between the toes to look whitish, overly soft, or waterlogged rather than simply dry.
- Burning, stinging, or discomfort – Beyond itch alone, the affected area might also feel sore, raw, or uncomfortable as the skin becomes more irritated.
- Weeping skin or fluid discharge – When the skin becomes more broken down, it might start to ooze or discharge fluid, especially in the irritated areas between the toes.
- An unpleasant odour – When the skin becomes damp, broken down, or weepy, some people might also notice a stronger smell coming from the affected area.
- Blisters in some cases – Some people might develop small fluid filled blisters, especially when the infection presents differently or the skin has become more irritated.
- Dry, scaly, or flaky skin – Fungal foot doesn’t only affect the toes, in some cases, other parts like the sole, sides, or heel might become drier and more prone to cracking.
Types of Fungal Foot
Fungal foot doesn’t always present in the same way. In some people, it stays mainly between the toes, while in others, it affects the sole, edges of the foot, or appears with more obvious blistering or skin breakdown. Because of that, understanding the main types of fungal foot can help explain why the condition might look different from one person to another.
Toe Web Infection
This is the most common type of fungal foot. It usually begins in the spaces between the toes, especially between the fourth and fifth toes, where moisture tends to stay trapped more easily. As the infection becomes more established, the skin in that area might start to break down and feel increasingly uncomfortable.
Moccasin Type Infection
This type follows a broader pattern across the bottom of the foot, often extending to the heel and outer edges. Rather than staying limited to the toe spaces, it tends to involve drier, more extensive skin changes across the sole. In less common cases, the toenails might also become involved, leading to fungal nail infection (onychomycosis).
Vesicular Type Infection
This form is defined by the presence of small fluid filled blisters and most often affects the bottom of the foot, although it might appear elsewhere as well. Because it presents differently from the patterns many people more commonly associate with fungal foot, it might not always be recognised straight away.
Ulcerative Infection
This is the rarest type of fungal foot and the most severe in how it affects the skin. Instead of remaining superficial, it involves deeper skin breakdown with open sores, also known as ulcers, which often appear between the toes or on the bottom of the foot. Because of that, it can be more painful and more concerning when it develops.
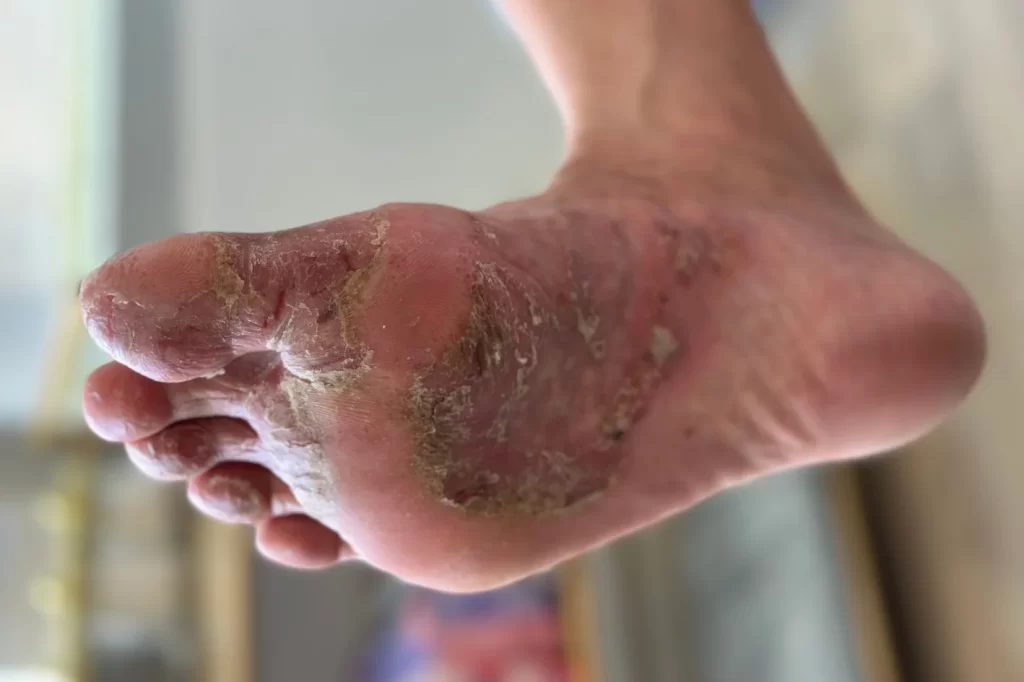
Need Help? See A Podiatrist Today
Causes of Fungal Foot
Fungal foot develops when certain fungi are given the right conditions to grow on the skin. Most often, this happens when the feet stay warm and damp for too long, or when the skin comes into contact with contaminated surfaces. In Singapore, this can become even more relevant during the south west monsoon period from June to September, when increased rain and humidity make it easier for moisture to linger around the feet.
What Causes Fungal Foot Infection?
- Dermatophyte fungi such as Trichophyton rubrum and Trichophyton interdigitale can multiply on the skin when conditions are favourable.
- The spaces between the toes tend to trap warmth and moisture more easily, which is why infection often begins there.
- Sweat that builds up inside socks and covered shoes can keep the skin damp for long enough to encourage fungal overgrowth.
- Wet socks, soaked shoes, and other forms of prolonged damp exposure can make it harder for the skin to dry properly.
- Humid and rainy conditions can increase the risk further by allowing moisture to linger around the feet for longer periods.
- Walking barefoot on contaminated communal surfaces such as poolside areas, locker rooms, and shared showers can increase direct exposure to fungi.
Who Is More Likely to Get Fungal Foot?
- Athletes and physically active individuals often spend long hours in sweaty footwear and might also use communal showers or changing areas more frequently.
- Military personnel and others who wear heavy boots for extended periods are more exposed to trapped heat, sweat, and poor ventilation around the feet.
- Workers in wet or humid environments might have feet that stay damp for much of the day, especially when rain, mud, or waterproof boots are involved.
- Swimmers and gym goers might come into more regular contact with damp communal surfaces where fungi can persist.
- People with excessive foot sweating (hyperhidrosis) are more vulnerable because constant moisture makes it harder for the skin to stay dry enough to resist infection.
- People with weakened immunity might be more susceptible because the body is less able to keep fungal infection in check.
Managing and Preventing Fungal Foot
Managing fungal foot usually involves treating the infection itself while also addressing the conditions that allowed it to develop in the first place. In many cases, this means reducing moisture, improving foot hygiene, and using antifungal treatment early so the infection is less likely to spread, become more stubborn, or keep returning.
Some common ways to manage fungal foot infection include:
- Applying topical antifungal creams in milder cases to help treat the fungal infection and settle the affected skin.
- Considering stronger prescription treatment in more persistent cases, which may include prescription strength topical medication or oral antifungal tablets.
- Using antifungal sprays or powders inside shoes where needed to help control moisture and reduce fungal build up in the footwear environment.
- Making footwear adjustments where needed so the feet aren’t kept warm, damp, and enclosed for longer than necessary.
- Discussing options such as Photodynamic Antimicrobial Therapy (PACT), in selected stubborn cases where more conventional treatment might not be enough.
To help reduce the risk of a returning fungal foot infection, it’s also worth paying closer attention to the daily habits that keep the feet dry and limit fungal exposure:
- Keep your feet clean and dry each day, especially after bathing, exercise, or long hours in covered footwear.
- Dry carefully between the toes, since moisture left behind there can make fungal growth easier.
- Choose socks that help wick moisture away from the skin, and change them when they become damp.
- Rotate your shoes regularly so each pair has time to dry fully before being worn again.
- Wear breathable or more open footwear where possible to reduce heat and moisture build up around the feet.
- Use slippers or shower shoes in communal areas such as gyms, pools, and shared showers to reduce direct contact with contaminated surfaces.
- Avoid sharing towels, socks, shoes, or other personal items that might harbour fungi, as this can allow the infection to spread.
When a fungal foot infection persists, doesn’t improve as expected, or starts affecting more of the foot, it’s worth having it properly assessed so the condition and any contributing footwear choice or lifestyle factors can be reviewed more clearly.
Have Your Fungal Foot Infection Managed at Straits Podiatry
Persistent fungal foot can be more disruptive than it first seems. The itching alone can become hard to ignore, while peeling, scaling, cracked skin, and ongoing irritation between the toes can make everyday comfort harder to maintain. In more established cases, the skin might start to soften from excess moisture, become weepy, or break down further, especially when scratching keeps aggravating the area. At Straits Podiatry, we will first assess whether your symptoms point to fungal foot and look more closely at how the infection is presenting, which parts of the foot are involved, and whether there are signs that the skin has become more damaged than expected.
Once we have a clearer picture of the issue, we can create a care plan tailored to your needs. This might include antifungal treatment, advice on keeping the feet drier, footwear guidance, and practical measures to reduce the risk of the infection lingering or returning. Speak with our team or book a consultation for an assessment and a tailored approach to manage your fungal foot infection.
Frequently Asked Questions About Fungal Foot Infection
How can I tell if my fungal foot is getting worse?
Your fungal foot might be getting worse when the itching becomes more persistent, the skin starts breaking down more noticeably, or the affected area becomes more painful, weepy, or widespread than before. More obvious cracking, a stronger odour, or changes that begin affecting the sole, sides, or heel can also suggest that the infection is becoming more established.
Can fungal foot infection spread to other parts of the foot or toenails?
Yes, it can. Although fungal foot often begins between the toes, it might also spread to the sole, sides, or heel. In some cases, the toenails might become involved as well, leading to fungal nail infection, also known as onychomycosis, which can cause the nails to thicken, become brittle, or change in appearance.
Is fungal foot contagious, and can it spread to other people?
Fungal foot can spread through contact with contaminated skin, shared personal items, or damp communal surfaces where fungi are able to persist. This is why shared showers, poolside areas, locker rooms, towels, socks, and footwear can all play a role in transmission, especially when the skin is already damp or broken down.
Why does my fungal foot keep coming back?
A fungal foot infection is more likely to return when the conditions that encouraged fungal growth haven’t been fully addressed. This can happen when the feet continue to stay damp, socks or shoes don’t dry properly, antifungal treatment is stopped too early, or there’s repeated exposure to communal wet areas. In some people, excessive foot sweating can also make recurrence harder to avoid.
When should my fungal foot be assessed professionally?
It’s worth having your fungal foot infection assessed by a podiatrist when it keeps returning, doesn’t improve as expected, starts affecting more of your foot, or leads to more significant skin breakdown. Assessment is also sensible when the area becomes increasingly sore, weepy, or uncomfortable, or when the toenails start showing signs of fungal infection as well.
Share this with someone you know



