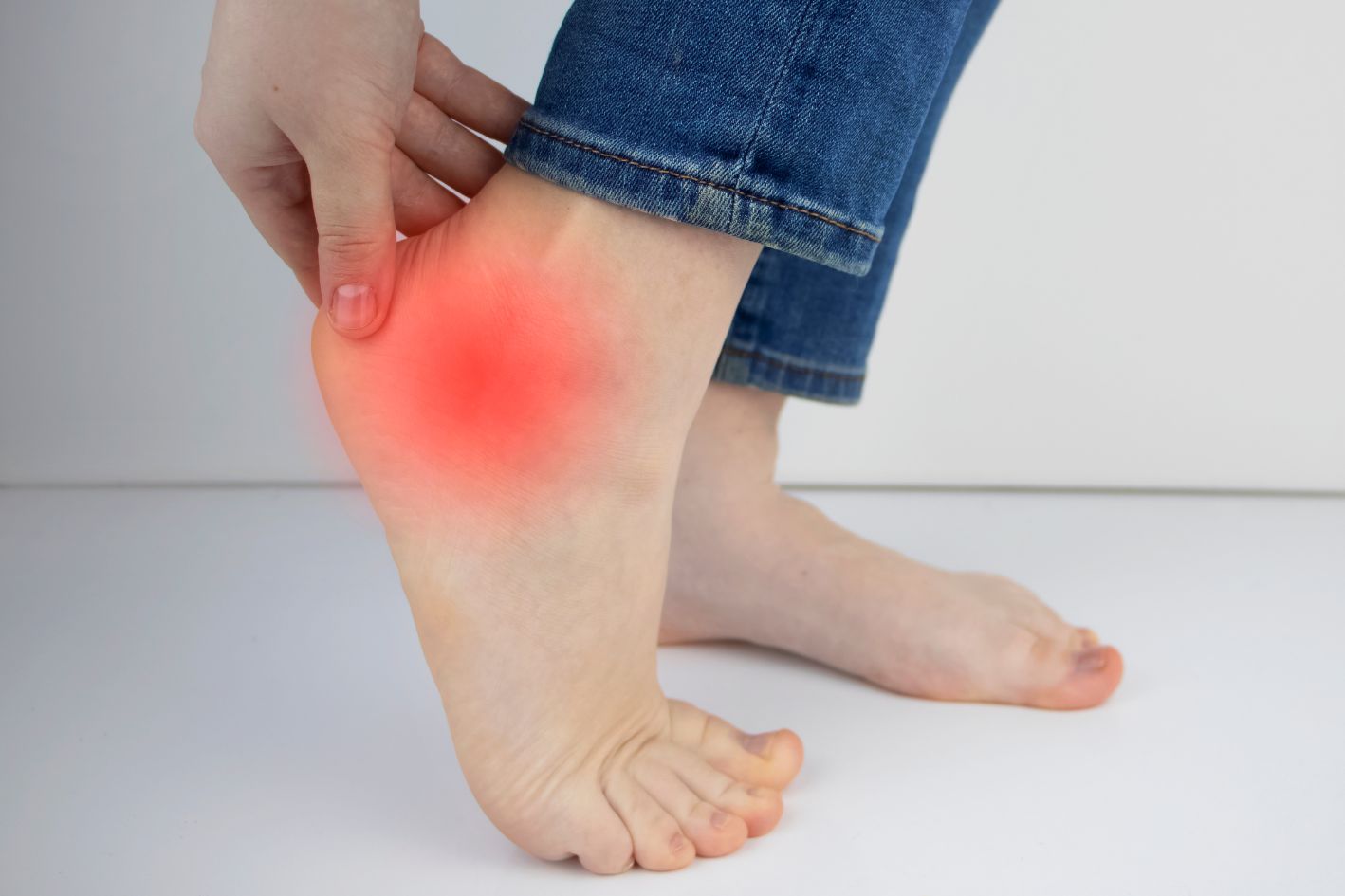
A nagging ache along the outer ankle or persistent soreness at the side of the foot can seem minor at first, especially when it only happens during walking, exercise, or long hours on your feet. Yet when it keeps returning in the same area, starts flaring under load, or lingers longer than expected, it becomes harder to dismiss as simple strain.
In some cases, this points to irritation of the peroneal tendons. These are the structures that run behind the outer ankle bone and along the side of the foot, where they help guide and steady movement. When they’re inflamed, repeated loading and motion can become more aggravating, which is why the problem often lingers rather than settles quickly.
This tendon problem is known as peroneal tendonitis. It often develops through overuse, although it can also happen after a fall or foot injury. Understanding the symptoms is an important next step in recognising how this condition presents and when it might require attention.
Symptoms of Peroneal Tendonitis
When the peroneal tendons become irritated, the symptoms usually begin around the outer ankle and will become more noticeable with activity. The following signs can help you recognise how peroneal tendonitis might present:
- Outer Ankle Pain – Pain is commonly felt around the outside of the ankle, especially near the outer ankle bone and along the tendon.
- Pain That Worsens with Activity – For those who are active, exercise or other forms of repetitive loading can make the discomfort more noticeable.
- Swelling, Redness, or Warmth – The area around the tendon might look swollen, appear red, or feel warmer than usual.
- Pain Along the Outer Foot – Pain can also extend along the outer border of the foot and might feel more intense than ordinary soreness, even when sedentary.
- Instability on Uneven Ground – The ankle might feel less steady (wobbly) when walking, especially on uneven surfaces.
- Poor Single Leg Balance – Standing on the affected side tends to feel more difficult, with a tendency to tip outward.
- Thickening or a Moving Nodule – In some cases, the tendon might feel thickened, or a small lump can be noticed moving with it.
- Gradual Onset – Symptoms often build over time and become more noticeable with continued activity.
Need Help? See A Podiatrist Today
Causes of Peroneal Tendonitis
Once the symptoms start becoming more noticeable, the next question is usually why the tendon has become irritated in the first place. In most cases, the answer lies in how much strain the peroneal tendons have been dealing with over time, as repeated loading can gradually outpace the body’s ability to recover. Still, this isn’t always a slow build, because an ankle sprain can also trigger a sudden bout of inflammation.
What Causes Peroneal Tendonitis?
- Repetitive overuse can gradually irritate the peroneal tendons when they are placed under more strain than they can recover from properly.
- Long periods of standing, walking, or running, especially after a sudden increase in activity, can place added stress on the tendons.
- An acute injury such as an ankle sprain can also trigger irritation or inflammation more suddenly.
- Poor training habits, including inadequate recovery between activities, can make it harder for the tendons to settle and repair.
- Weakness or tightness in the muscles of the foot or leg can alter how load moves through the area and place more strain on the tendons.
- Unsupportive footwear might reduce stability around the foot and ankle, making the tendons work harder.
Who Carries a Higher Baseline Risk?
- Ageing is associated with a higher risk of tendon problems, which is why peroneal tendonitis is more often seen after the age of 40.
- Being overweight can increase the amount of load passing through the foot and ankle and place more stress on the tendons.
- People with high arches (Pes cavus) are more prone because of how force is distributed along the outer side of the foot.
- Certain medical conditions such as diabetes, rheumatoid arthritis (RA), osteoarthritis (OA), and gout, might increase the likelihood of tendon related problems.
- A history of previous foot or ankle trauma, tendon injury, or surgery might leave the area more vulnerable.
- Smoking has been associated with poorer tendon health and might increase the risk of tendon problems.

Managing and Preventing Peroneal Tendonitis
Managing peroneal tendonitis usually starts with reducing irritation around the tendon and giving the area a chance to settle. In many cases, conservative care is enough to ease pain and inflammation within a few weeks, although recovery can take longer when the problem is linked to another injury such as an ankle sprain.
Some common ways to manage peroneal tendonitis include:
- Reducing or pausing the activities that keep aggravating the tendon, especially running, jumping, or repeated loading through the foot and ankle.
- Using the RICE method at home with rest, ice, compression, and elevation to help manage pain and swelling.
- Wearing an ankle brace or, in some cases, a boot to support the area and reduce strain while the tendon settles.
- Taking anti-inflammatory medication such as non-steroidal anti-inflammatory drugs (NSAIDs) if advised, to help relieve pain and inflammation.
- Going for physiotherapy to improve strength, flexibility, and control around the foot and ankle as recovery progresses.
- Following a care plan tailored to the severity of the irritation and whether another injury is involved.
To help reduce the risk of the problem returning, it’s also worth paying closer attention to the habits and factors that might keep overloading the tendons:
- Build up activity levels gradually rather than increasing intensity too quickly.
- Make room for proper recovery between workouts, games, or other repeated physical activity.
- Warm up the feet and ankles before exercise, especially before higher impact movement.
- Avoid pushing through foot or ankle pain when symptoms start to return.
- Wear supportive footwear, and use additional support such as custom orthotics.
- Maintain a healthy body weight and avoid smoking, as both can affect the amount of strain on the area and how well the tendons recover.
When pain along the outer ankle keeps returning despite these measures, or starts affecting balance, activity, or daily movement more, it’s recommended that you have the problem assessed properly by a podiatrist so that the right care plan can be considered.
Have Your Peroneal Tendonitis Managed at Straits Podiatry
When pain along the outer ankle or side of the foot keeps returning, it can begin to affect far more than exercise alone. Walking, standing for longer periods, and even moving across uneven ground will start to feel less steady or comfortable than they should. At Straits Podiatry, we will first assess whether your symptoms point to peroneal tendonitis, examine how the tendon is coping with load and movement, and look at the factors contributing to the condition.
Once we have a clearer understanding of what’s behind your discomfort, we can map out a care plan tailored to your needs. This might include activity modification, footwear advice, support to reduce strain on the tendon, and targeted care to help the area settle better. Speak with our team or book a consultation for an assessment and a tailored approach to manage your peroneal tendonitis.
Frequently Asked Questions About Peroneal Tendonitis
Is peroneal tendonitis the same as peroneal tendinitis, and how is it different from tendinopathy?
Peroneal tendonitis and peroneal tendinitis refer to the same condition, with the difference simply being how the word is spelt. Tendinopathy is broader. It’s a catch all term used for conditions affecting the tendon, including tendinitis, tendinosis, and tenosynovitis. So, while peroneal tendonitis is a specific tendon problem, peroneal tendinopathy is the wider term you might also come across when you search online for answers to your ankle tendon pain.
Can peroneal tendonitis be mistaken for an ankle sprain?
Yes, it can, especially when pain is felt around the outer ankle after activity or following a twist. Both can cause discomfort, tenderness, and difficulty walking comfortably. However, peroneal tendonitis involves irritation of the tendon, while an ankle sprain affects the ligaments. If the pain keeps returning, feels linked to loading, or doesn’t settle as expected, proper assessment by a podiatrist helps clarify what structure is actually involved.
Can high arches contribute to peroneal tendonitis?
Yes, they can. People with high arches will tend to place more load along the outer side of the foot, which can increase strain on the peroneal tendons over time. This doesn’t mean everyone with high arches will develop peroneal tendonitis, but it can raise the baseline risk. In some cases, footwear changes or podiatry guided orthotic management for better support might help reduce repeated stress through the area.
Can footwear choice or custom orthotics help with peroneal tendonitis?
They can in the right situation. Supportive footwear helps reduce unnecessary strain on the peroneal tendons, especially if unsupportive shoes are making the problem worse. Custom orthotics can also be useful for some people, such as those with high arches or biomechanical factors that increase load along the outer foot. However, they should be recommended based on assessment by a podiatrist rather than replaced with a pair of off-the-shelf insoles that are not matched to how your foot is loading.
Does peroneal tendonitis always need surgery?
No, not always. Peroneal tendonitis is often managed without surgery, particularly when it’s identified early and the tendon is given a chance to settle with the right form of podiatry care. Management would include load modification, supportive footwear, physical therapy, and other conservative measures. Surgery is only considered when symptoms persist, structural damage is suspected, or the problem doesn’t improve with appropriate non-surgical care.
Share this with someone you know