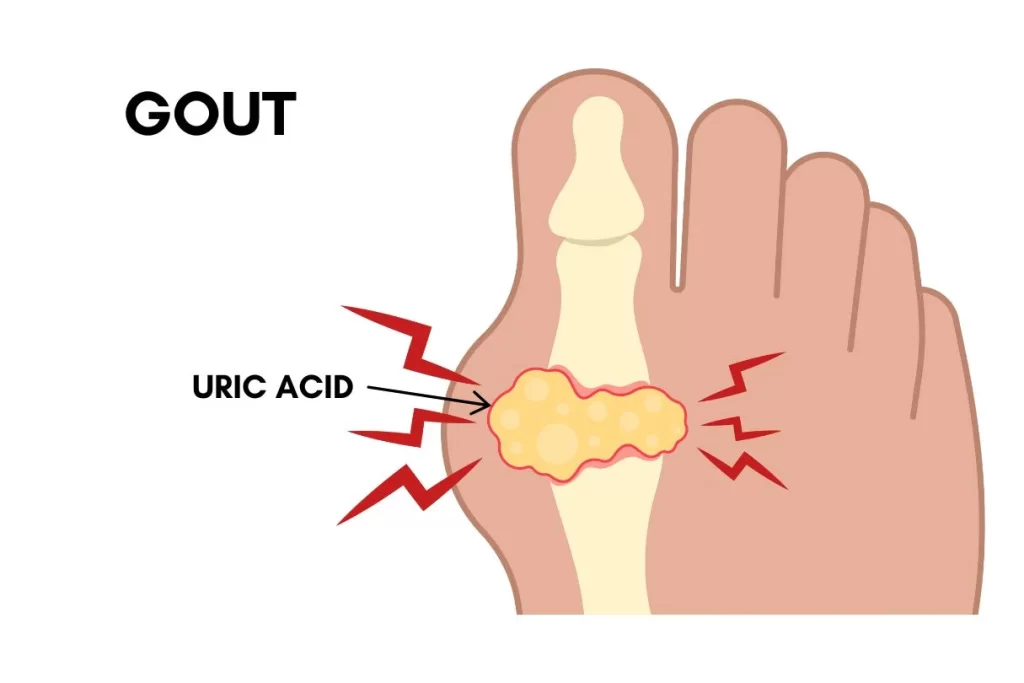
A gout flare often strikes at the worst time. You go to sleep feeling normal, then all of a sudden wake in the middle of the night with a burning pain in the foot or ankle that feels extreme for such a small joint. The area can swell, turn hot, and become so sensitive that even light contact feels unbearable, which is why the pain often feels shocking the first time it hits.
For many, the big toe joint is where gout shows up first (podagra). Yet it can also flare in the ankle or other parts of the foot, and the effect on mobility is immediate. When one side hurts, you can still limp and protect it, but when both feet are involved at the same time, there is no “good” side to rely on, and this makes a short trip to the bathroom an ordeal.
To understand why it hits this hard, it helps to know what is happening inside the joint. Gout is driven by intense inflammation triggered by uric acid crystal build up, which is why it often arrives as a sudden flare rather than a slow build. With that foundation set, the next section breaks down the symptoms of gout and how they typically present.
Symptoms of Gout
Gout symptoms often come on suddenly and escalate fast. It can start as a warm, throbbing sensation in a joint, then intensify into sharp pain that makes even small movements difficult. Although a flare can ease within a week, the joint often stays sensitive for longer, especially if you are still walking on it. Gout most commonly affects the big toe joint, but it can also affect the foot, ankle, and knee.
- Intense joint pain – Pain often peaks within the first four to 12 hours, and weight bearing can feel difficult or even impossible.
- Lingering discomfort – Even after the sharpest pain settles, soreness can persist for days or weeks, and repeated attacks often last longer.
- Inflammation and tenderness – The joint can become swollen, warm, and red, while the surrounding skin feels tender and highly sensitive to touch.
- Reduced movement and stiffness – Range of motion can tighten during a flare, making the joint feel stiff, guarded, and harder to move normally.
The Four Stages of Gout
Gout is often thought of as a sudden attack in the big toe, but it usually develops in stages. Some phases are silent, while others are painful and disruptive, which is why gout can feel like it “comes and goes” even when the underlying problem is still present.
First Stage: Asymptomatic Gout
In the initial stage, uric acid gradually builds up in the blood (hyperuricemia). During this time, urate crystals can begin forming in and around joints, yet there are no obvious symptoms. Because nothing feels wrong, this stage often goes unnoticed, even though the groundwork for future flare ups is already being laid.
Second Stage: Acute Gout
Over time, crystal build up triggers a sudden inflammatory response, leading to an acute gout flare. This is when pain hits sharply, often with swelling, heat, and redness around the joint. The discomfort can peak quickly and make weight bearing difficult, which is why many people describe it as an attack that appears out of nowhere.
Third Stage: Intercritical Gout
After the flare settles, symptoms can disappear completely, creating a symptom free window known as intercritical gout. Even so, the underlying crystal deposits can remain, and uric acid levels can still stay high in the background. This explains why gout can feel quiet for months or years, then return with another flare when the joint is triggered again.
Fourth Stage: Chronic Tophaceous Gout
If gout stays uncontrolled over time, it can progress into a more persistent form. Larger deposits of urate crystals, known as tophi, can develop in joints and soft tissues, leading to ongoing pain, stiffness, and joint damage. At this stage, movement can become more restricted, and complications such as kidney stones can also become part of the picture.
Need Help? See A Podiatrist Today
Causes of Gout
With gout, the main issue is not one specific trigger, but the uric acid level your body carries in the background. When uric acid stays elevated, crystals can build up quietly around joints over time, which is why flare ups can return in cycles even when you feel fine between attacks. From there, certain lifestyle factors, medical conditions, and medications can push uric acid higher or make it harder for the kidneys to clear it, increasing the likelihood of another flare.
What Increases Uric Acid Levels?
- Purine rich foods such as red meat, organ meats, and some seafood can raise uric acid as the body breaks down purines.
- Sugary drinks, especially those high in fructose, can increase uric acid levels.
- Alcohol, especially beer, can increase uric acid and raise the chance of flare ups.
- Reduced kidney function can make it harder for the body to remove uric acid efficiently.
- Certain medications, especially some diuretics and low dose aspirin, can raise uric acid levels by affecting how the kidneys clear it.
Who Carries Higher Baseline Risk?
- Men are more likely to develop gout earlier, often between the ages of 30 and 50.
- Women can also get gout, and risk rises after menopause as uric acid levels increase closer to men’s levels.
- People who are overweight often carry higher uric acid levels and face higher gout risk.
- People with conditions such as high blood pressure, diabetes, heart disease, or kidney disease tend to have a higher baseline risk.
Conditions Commonly Mistaken for Gout
Because gout often presents as sudden, intense pain with swelling and redness around the big toe joint, it can be confused with other conditions that affect the same area. While the symptoms might feel similar at first, the cause behind them is often different, which is why getting the diagnosis right matters.
- Bursitis – Inflammation of soft tissue cushioning near the joint can cause local pain and swelling that feels similar to gout. However, bursitis is centred around the surrounding tissue rather than being caused by uric acid crystal inflammation within the joint.
- Bunions – Bunions are bony bumps at the base of the big toe that often cause soreness, swelling, and redness, especially in shoes. Unlike gout, which often flares suddenly with intense pain and inflammation, bunions are linked to joint misalignment and develop gradually over time.
- Hallux rigidus – Hallux rigidus (osteoarthritis) involves wear and stiffness within the big toe joint, often causing pain during toe bend and reduced movement. Gout tends to cause more abrupt flare ups with intense joint pain, swelling, warmth, and tenderness.
- Sesamoiditis – This causes pain under the big toe joint, and it often worsens with walking and push off through the forefoot. Unlike gout, which often strikes suddenly with intense pain, swelling, redness, and tenderness, sesamoiditis usually builds gradually from repeated pressure rather than appearing overnight.
- Pseudogout – Pseudogout can cause sudden pain, swelling, warmth, and redness around a joint, and it can sometimes be mistaken for gout when symptoms flare near the big toe region. Unlike gout, which is driven by uric acid crystal deposits, pseudogout is driven by inflammation triggered by calcium pyrophosphate crystal deposits.
Managing and Preventing Gout
Once gout becomes a recurring issue, the focus shifts from getting through one flare to lowering how often the attacks return and how disruptive they feel when they hit. This works best when pain is managed early, while the long-term drivers behind high uric acid are addressed concurrently. Over time, this protects joint comfort and helps walking feel more normal again.
To begin, focus on settling the flare and reducing stress on the joint while it is at its most sensitive:
- Resting the affected foot and reducing weight bearing until the pain eases.
- Using cold packs briefly to ease pain and swelling during severe flare ups.
- Short term medication such as non-steroidal anti-inflammatory drugs (NSAIDs) or corticosteroids, where appropriate and guided by your doctor, to manage inflammation and pain.
- Target drug therapy, such as Colchicine, may also be prescribed by your doctor to manage recurring acute inflammation.
Next, focus on reducing the likelihood of repeat flare ups by keeping uric acid levels more stable over time:
- Avoiding crash diets, long fasts, and skipped meals, since ketone spikes and dehydration can aggravate inflammation and make flare ups more likely.
- Keeping weight changes gradual where possible, since sudden shifts can destabilise uric acid control.
- Reducing high purine foods such as organ meats, red meat, and some seafood.
- Cutting back on alcohol, especially beer, and limiting sugar sweetened drinks that are high in fructose.
If flare ups keep returning despite consistent lifestyle adjustments, additional non-invasive support can be considered as part of a broader plan:
- Extracorporeal Shockwave Therapy (ESWT) can be discussed to help reduce pain and support recovery in the affected joint.
- Custom orthotics can help to address foot biomechanics, especially if you are flat footed or high arched, as joint stress can trigger gout attacks
Finally, prevention is about keeping things steady rather than perfect. This means returning to activity in stages after a flare, keeping daily habits consistent, and avoiding sudden spikes in load through the feet. Stress also matters, because prolonged strain and poor sleep can raise cortisol and adrenaline, which keeps the body in a more reactive state and makes flare ups harder to settle. With the right structure in place, flare ups can feel more manageable and daily movement often becomes less disrupted.
Have Your Gout Pain Managed at Straits Podiatry
When gout strikes, it can turn a normal day into a struggle to walk comfortably, especially when the big toe, foot, or ankle is the joint taking the hit. At Straits Podiatry we first confirm whether your symptoms match the flare pattern of gout, then assess how the joint is coping with load through daily movement. Where useful, ultrasound imaging can also help us review the joint area more closely.
Once we have a clearer view of what is driving your flare cycle, we will then map out a personalised plan for you. This can include footwear adjustments to reduce irritation, simple pacing strategies to prevent pain from spiking when you walk or stand too much, and guidance to reduce pressure through the foot while the joint settles. If pain persists, ESWT can also be arranged as part of your care plan. Speak with our team or book a consultation for an assessment and a tailored approach to manage your gout pain.
Frequently Asked Questions About Gout
What is gout and what causes it?
Gout is an inflammatory arthritis driven by uric acid imbalance. When uric acid stays elevated, sharp urate crystals can form in and around a joint, which then triggers a strong inflammatory response. Uric acid comes from breaking down purines through normal metabolism and certain foods. So, when the body produces too much uric acid or clears too little of it, crystals can accumulate and the likelihood of flares becomes higher.
How do I know if the pain I have is gout?
Gout pain often strikes suddenly and feels sharp and intensely tender, and it commonly affects the big toe, foot, or ankle. The joint can swell, look red, and feel warm to the touch, and even light contact with a blanket can feel unbearable. Because it escalates quickly, walking can become difficult within hours. If this pattern repeats, an assessment helps confirm whether gout is the true cause.
What can a podiatrist do for my gout?
A podiatrist can assess the joint, check your symptom pattern, and then determine whether the pain fits gout or another foot condition. Where applicable, ultrasound imaging can help evaluate the area more closely. Care then focuses on protecting the joint during flares with footwear guidance and activity pacing, so walking feels more manageable while it settles. If pain remains stubborn, ESWT and custom orthotics can also be discussed as supportive care.
How does ESWT help relieve gout pain?
ESWT supports pain relief by improving local circulation and influencing how tissue responds to stress. Through mechanotransduction, mechanical pressure is converted into biological signals that support recovery processes. As a result, angiogenesis can be stimulated, improving blood flow to reactive tissue. In addition, collagen synthesis can be encouraged, supporting tissue resilience over time.
Can gout cause long term joint damage or affect the kidneys?
Yes. When gout keeps recurring or stays uncontrolled, repeated inflammation can contribute to joint damage, stiffness, and reduced movement over time. Beyond the joints, gout is also linked to kidney issues because uric acid can form crystals in the urinary system, which increases the risk of kidney stones and can affect kidney function. For that reason, long term control matters, not only flare relief.
Share this with someone you know