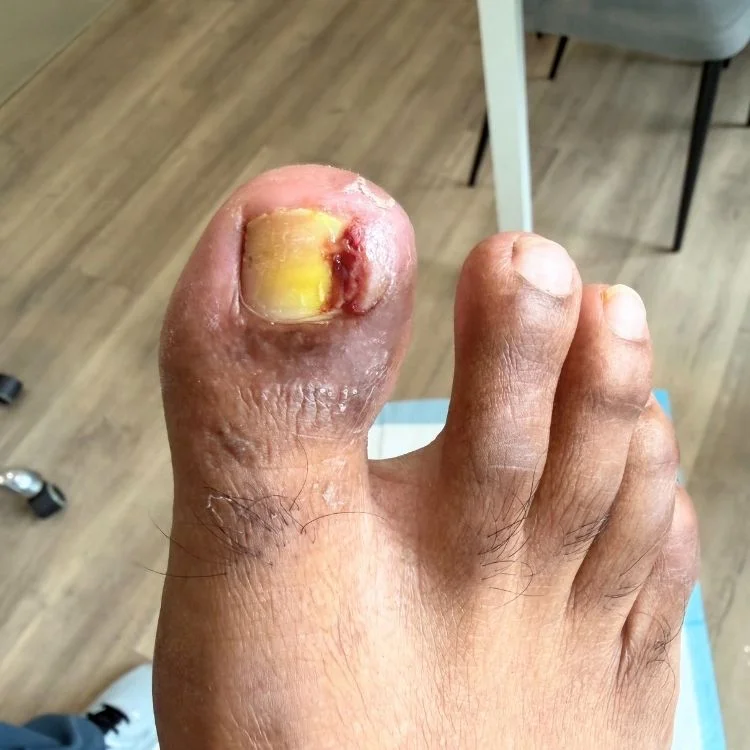
Returning to Running After Peroneal Tendonitis: What Recovery Actually Looks Like

Getting back to running or sport after peroneal tendonitis is one of the questions patients like to ask podiatrists, much like other musculoskeletal problems, and it rarely gets a satisfying answer from a quick search. The timelines people find online range from two weeks to six months, which is not particularly helpful when you have a race on the calendar or a badminton session you have already postponed twice.
Unfortunately, there is no standard way to answer it. The truth is that recovery time depends on how irritated the tendon is, how long it has been symptomatic, and critically, how the return to activity is structured.
Returning too soon is the most common reason peroneal tendonitis lingers far longer than it needs to. Understanding why that happens, and what a more structured approach looks like, makes the difference between a problem that resolves in weeks and one that keeps resurfacing for months.
Why Tendons Take Longer Than Muscles to Recover
Most people understand intuitively that a muscle strain gets better faster than a bone injury. Tendon injuries sit somewhere in between, and the reason matters for how you approach recovery.
Tendons have a relatively poor blood supply compared to muscle tissue. Blood flow is how the body delivers the building blocks needed for tissue repair, so less blood flow means slower healing. When a tendon is irritated and inflamed, the initial response happens reasonably quickly. Swelling and pain often settle within a few days of reducing activity. But this does not mean the tendon has recovered its structural capacity. The tissue is still in the process of remodelling, which continues for weeks after symptoms subside.
This is the trap most active people fall into. The pain goes away, they return to full training, and the peroneal tendon, which has not yet rebuilt its capacity to handle that load, breaks down again. The cycle repeats, and what started as a three-week problem becomes a four-month one.
The peroneal tendons specifically run behind the outer ankle bone and bear significant load during any activity involving push-off, lateral movement, or uneven surfaces. In people with high-arched feet, this load is even more pronounced because of how force is distributed along the outer border of the foot. The tendon needs to be progressively loaded to genuinely recover, not simply rested until it stops hurting.
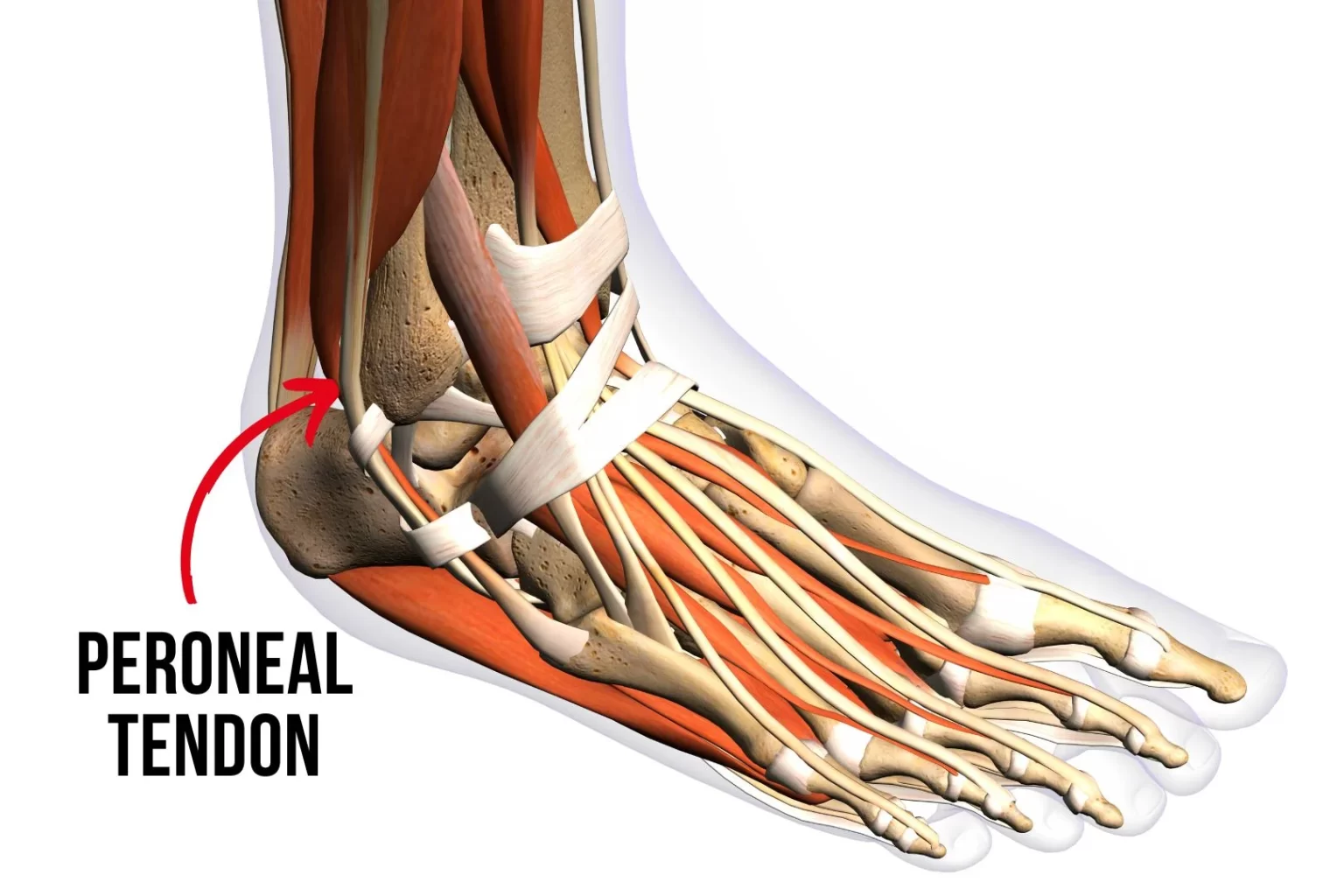
What Realistic Recovery Actually Involves
There is no single timeline that applies to everyone, but there are predictable phases that most people move through. Where you start depends on how irritated the tendon is when you begin structured recovery. Here’s what you can expect if you are suffering from an acute peroneal tendonitis that has just occurred. Bear in mind that if you have been suffering from the issue for months, recovery may involve more treatment options.
Phase 1: Settling the Irritation (Days 1 to 14)
The priority in the first phase is reducing the inflammatory load on the tendon. This means modifying or pausing the activities that aggravate it, particularly running, jumping, and sustained court sports. It does not necessarily mean complete rest from all movement.
During this phase, low-load activities that maintain general fitness without stressing the peroneal tendon are appropriate for most people. Swimming, cycling on a stationary bike, and upper-body strength work are typically well tolerated. Walking on flat, even surfaces is usually fine.
Ice applied to the outer ankle after any activity that causes mild discomfort helps manage local inflammation. Compression and elevation when at rest reduce swelling. If you are continuing any weight-bearing activity, footwear matters considerably during this phase. A shoe with good lateral support and a moderate heel-to-toe drop reduces the demand on the peroneal tendons compared to minimalist or worn-out trainers.
Phase 2: Rebuilding Tendon Capacity (Weeks 2 to 6)
Once pain at rest has resolved and discomfort with gentle daily activity has settled, progressive loading of the tendon can begin. This is the phase most people either skip entirely or do too aggressively.
Progressive loading works by applying controlled stress to the tendon in gradually increasing amounts. The tendon responds to this stimulus by remodelling its collagen fibres into a more organised, load-bearing structure. Without this stimulus, the tendon heals but does not rebuild the structural resilience it needs for sport.
Practically, this means beginning with exercises that load the peroneal muscles and tendons in a controlled way: seated resistance band eversion, standing calf raises progressing to single-leg, and gradual introduction of balance and proprioception work on an unstable surface. Each progression should be guided by how the tendon responds over the following 24 hours. Mild awareness of the tendon after exercise is acceptable. Pain that persists into the next day is a signal to step back.
Walking duration and pace can increase through this phase. Light jogging on flat surfaces is typically introduced toward the end of Phase 2 for people who are progressing well, starting with short intervals separated by walking.
Phase 3: Return to Sport-Specific Load (Weeks 6 to 12)
The final phase is where activity becomes genuinely sport-specific again. For runners, this means progressive increases in weekly mileage, introduction of varied terrain, and eventually faster pace work. For court sport players, it means lateral movement drills, direction changes, and sport-specific footwork before returning to match play.
The 10% rule is a useful rough guide: total weekly load should not increase by more than approximately 10% from one week to the next. This applies to running mileage, training duration, and the intensity of court sessions. Jumping to full training after a period of reduced activity is the most reliable way to provoke a recurrence.
By the end of this phase, most people with a well-managed peroneal tendonitis are back to full activity. Some with more significant or long-standing tendon involvement take longer, particularly if the tendon has developed structural changes rather than simple inflammation.
Need Help? See A Podiatrist Today
Sport-Specific Considerations in Singapore
Runners
Singapore has a large and active running community, and the pressure to get back to training, particularly when a race entry has already been paid for, is real. The most important thing to understand is that returning to running before the tendon has rebuilt its capacity does not shorten the overall recovery window. It extends it, often significantly.
Trail running and uphill routes are the last elements to reintroduce, even after flat road running feels comfortable. The lateral demands of uneven terrain and the eccentric loading on descents place substantially more stress on the peroneal tendons than flat road running at the same pace. The Standard Chartered Singapore Marathon course is predominantly flat, which is helpful. Races involving MacRitchie or the Southern Ridges are considerably more demanding on the outer ankle.
For runners whose ankle sprains triggered their peroneal tendonitis, the return-to-running timeline may be slightly longer because both the ligaments and the tendon need sufficient recovery before full load is appropriate.
Badminton, Basketball, Tennis, Pickleball
Lateral movement, rapid direction changes, and explosive push-off are the actions that put the greatest demand on the peroneal tendons. For court sport athletes, this means that being pain-free during straight-line jogging does not reliably indicate readiness for match play.
A more useful test is the lateral shuffle: moving sideways at increasing speed without provocation of symptoms. Single-leg calf raise endurance, tested by counting repetitions to fatigue on the affected side versus the unaffected side, also gives a practical indication of whether the tendon has regained sufficient capacity. A deficit of more than 20% between sides suggests the tendon is not yet ready for the lateral demands of match play.
Returning to drills before returning to match play, and to match play before full competition, gives the tendon the graduated exposure it needs without the unpredictable load spikes of competitive sport.
Gym Training and Resistance Work
Lower body resistance training can generally resume earlier than running or court sport, because controlled bilateral exercises place less dynamic and lateral demand on the peroneal tendons. Squats, leg press, and deadlifts are typically well-tolerated in Phase 2, provided the tendon is not being loaded in a provocative range. Single-leg and lateral exercises, such as lateral lunges and single-leg Romanian deadlifts, are introduced progressively in Phase 3.
Red Flags During Return to Activity
Most people will experience some level of discomfort in the tendon during recovery, and this is not cause for alarm. The signals that indicate you are moving too fast include:
- Pain or significant soreness that persists more than 24 hours after a session
- Swelling that increases after activity rather than remaining stable or decreasing
- Onset of the original pain during the activity itself, rather than only after
- A returning sense of instability or giving way at the outer ankle
- Pain at rest returning after it had previously settled
If any of these occur, the appropriate response is to step back one phase rather than stopping completely. Complete rest at this stage is generally not necessary and interrupts the remodelling process that the tendon needs to progress.
Remember, all rehabilitation journey have some setbacks along the way, and it is very normal.

The Role of Footwear and Orthotics in Recovery
Footwear is key in peroneal tendonitis recovery. Shoes that lack lateral support, have excessive heel drop, or are worn through at the outer heel place additional rotational stress on the ankle and increase the load the peroneal tendons have to manage with every step.
During recovery, a shoe with a firm, supportive midsole, adequate toe box width, and moderate heel counter is preferable to minimalist or highly cushioned footwear that sacrifices stability. Court sport shoes designed with lateral support are generally appropriate for badminton and tennis players returning to training.
For people whose peroneal tendonitis is related to foot structure, particularly those with high-arched feet or biomechanical factors that increase outer ankle load, custom sports orthotics can meaningfully reduce the demand on the peroneal tendons during activity. These are best assessed and prescribed as part of a broader management plan rather than purchased over the counter.
When Recovery Is Taking Longer Than Expected
Some people do everything right and still find that peroneal tendonitis is not resolving on a typical timeline. There are a few reasons this happens.
Tendon changes that have moved beyond simple inflammation into structural degeneration (tendinosis) take longer to respond to progressive loading and may require additional input. In these cases, regenerative therapies can help stimulate the remodelling process more effectively.
Focused shockwave therapy is one approach used for persistent tendon conditions that have not responded adequately to conservative management alone. It works by delivering targeted acoustic energy to the affected tendon, stimulating a localised healing response in tissue that has become slow to remodel on its own.
It is also worth considering whether the underlying biomechanical factors contributing to the tendonitis have been properly addressed. If the load distribution through the foot and ankle has not changed, the tendon is under the same stressors that caused the problem in the first place, regardless of how carefully the return to activity has been managed.
Getting the Assessment Right From the Start
The most reliable way to avoid an extended recovery is to have the tendon properly assessed before loading it back up. Understanding the degree of irritation, whether any structural tendon changes are present, and how foot mechanics are contributing to the problem gives a much clearer basis for the return-to-activity plan.
At Straits Podiatry, establishing a full clinical picture helps plan your peroneal tendonitis treatment, including how the return to activity is structured and monitored. Our podiatrists will provide a detailed assessment and design a tailored management plan to meet your goals.
If you are currently managing outer ankle pain and are unsure whether it is ready for sport, or if a previous episode has not settled as expected, a podiatry consultation gives you a clear assessment of where the tendon is in its recovery and what is appropriate from that point.

Jackie Tey
Chief Podiatrist, B.Pod(Hons). Your foot and lower limb specialist passionate about raising awareness for foot and lower limb health.