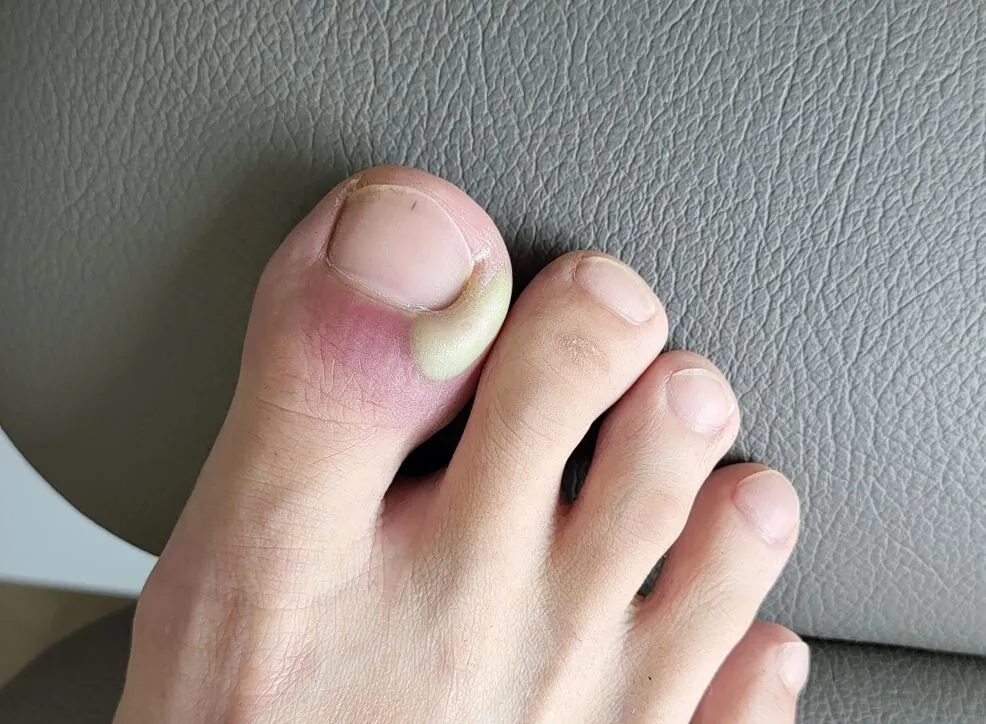
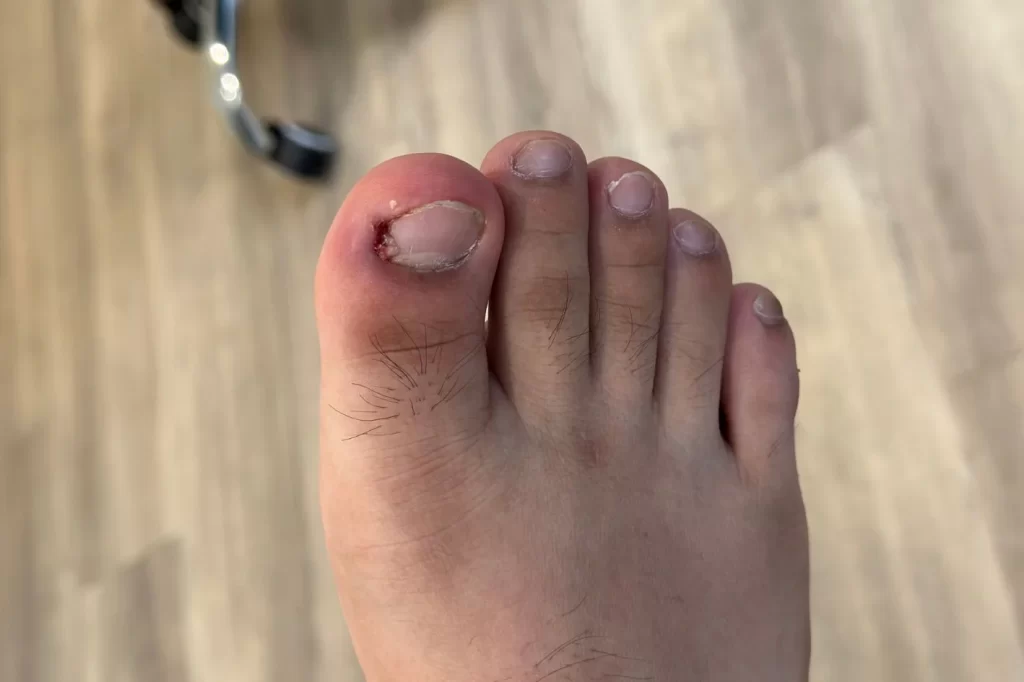
The soreness might begin as a faint tenderness at the corner of your toenail that you notice when lacing up your shoes or stepping on an uneven surface. Within a day or two, the skin alongside the nail edge becomes visibly red, warm to the touch, and swollen enough to make your sock feel tight. Pressing on that strip of skin produces a sharp, localised ache, and you may notice a small pocket of pus beginning to collect beneath the surface. It is easy to dismiss this early as a minor irritation, but once an infection takes hold in that tissue, it does not reliably resolve without some form of care.
The tissue that sits directly alongside and above your nail is called the nail fold, and the full region surrounding the nail plate on three sides is known as the perionychium. In a healthy nail, a thin layer of skin called the cuticle forms a tight seal between the base of the nail plate and the nail fold behind it. This seal keeps bacteria and fungi out of the soft tissue below. The cuticle is not cosmetic. It is a functional barrier. When that barrier is broken, whether by trauma, aggressive cutting during a pedicure, or prolonged moisture softening the skin, microorganisms have a direct entry point into tissue that is warm, moist, and receives relatively little airflow.
Paronychia is the term for infection or inflammation of this periungual (nail fold) tissue. It traditionally falls into two broad categories: acute paronychia, which develops rapidly over hours to a couple of days and is typically driven by bacteria; and chronic paronychia, which builds slowly over several weeks or more and is more commonly linked to fungal organisms, particularly Candida species. A third pattern is increasingly recognised in clinical practice: drug-induced paronychia, particularly from certain chemotherapy and targeted cancer therapies, which causes nail fold changes as a direct medication side effect rather than from primary microbial infection. All three forms affect the toenails, and the same nail fold anatomy that makes toenails susceptible to ingrown toenails is also the site where paronychia develops.
Symptoms of Paronychia
Acute and chronic paronychia produce overlapping but distinguishable presentations. Acute paronychia tends to arrive sharply, with symptoms escalating over a short period, while the chronic form lingers at a lower intensity without fully settling.
In acute paronychia:
- Redness and warmth along the nail fold – the skin beside and behind the nail edge becomes flushed and noticeably warmer than the surrounding tissue
- Localised swelling – the periungual skin thickens and lifts slightly, which can make footwear press uncomfortably against the toe
- Tenderness on direct pressure – pressing the nail fold, or even light contact with a sock or shoe, produces a sharp, localised ache
- Pus accumulation – in more developed cases, a visible pocket of creamy or yellow-white fluid collects just beneath the skin surface near the nail margin
- Throbbing pain – as pressure builds within the confined tissue, the pain may take on a pulsating quality, noticeable even without direct contact
In chronic paronychia:
- Persistent low-level tenderness – the nail fold remains mildly sore for weeks at a time without clearly resolving or worsening
- Cuticle recession or loss – the cuticle progressively breaks down as chronic inflammation weakens the tissue, removing the seal that protects the nail fold
- Nail plate changes – the nail may develop horizontal ridges, surface irregularities, or subtle discolouration as the sustained inflammation near the nail base disrupts normal growth
- Moist or boggy periungual skin – the tissue surrounding the nail feels slightly swollen and soft rather than firm, and may appear pale or macerated from repeated moisture exposure

Types of Paronychia
Acute Paronychia
Acute paronychia develops over hours to a few days and is almost always driven by bacteria, most commonly Staphylococcus aureus or Streptococcal species, entering through a break in the periungual skin. The infection is typically confined to the nail fold itself and does not extend into the deeper tissue below. Without intervention, bacterial colonisation can progress to abscess formation, where pus accumulates in a pressurised pocket beneath the skin surface. In the foot, acute paronychia frequently occurs alongside or as a direct consequence of an ingrown toenail, where the nail edge creates a wound channel that gives bacteria a reliable route into the tissue.
Chronic Paronychia
Chronic paronychia is defined by a duration of six weeks or more and a pattern of repeated low-grade inflammation rather than a single acute episode. The underlying driver is most often fungal, particularly Candida albicans, and the condition is closely linked to environments where the feet remain wet for extended periods. As episodes repeat, the cuticle breaks down progressively, meaning the barrier that would otherwise contain future infections continues to deteriorate. Nail plate changes, including ridging and discolouration, are more common in chronic cases because the sustained inflammation at the nail matrix level interferes with normal nail production. Chronic paronychia may also develop from repeated acute episodes that were not fully resolved.
Chemotherapy-Related (Drug-Induced) Paronychia
Several classes of anti-cancer medication can cause paronychia as a side effect rather than as a primary bacterial or fungal infection. This pattern has become increasingly recognised as targeted cancer therapies have become more widely used. The drugs most commonly implicated include EGFR inhibitors (such as cetuximab, panitumumab, gefitinib, erlotinib, and afatinib), taxanes (docetaxel, paclitaxel, nab-paclitaxel), tyrosine kinase inhibitors, BRAF and MEK inhibitors, and oral retinoids used in certain cancer and dermatological protocols.
The typical onset is 4 to 12 weeks after starting therapy. What distinguishes this form from bacterial or fungal paronychia is the pattern: multiple nails are often affected at the same time, commonly involving both fingernails and toenails bilaterally rather than a single digit. A further distinctive feature is the frequent development of periungual pyogenic granulomas, which appear as bright red, fleshy, cauliflower-like overgrowths of tissue at the edge of the nail fold that bleed easily on contact. The nail fold itself becomes inflamed and swollen, and secondary bacterial infection can develop on top of the underlying drug-induced changes.

Causes of Paronychia
Paronychia requires two conditions to develop: a break in the periungual skin barrier and the presence of microorganisms that can exploit that breach. In most cases the break is not dramatic. It results from everyday habits or exposures that gradually weaken the protective tissue around the nail.
什么原因导致甲沟炎?
- Ingrown toenail – when the nail edge presses into the nail fold, it creates a persistent wound channel where bacteria can enter and establish infection, often making the paronychia recurrent until the nail position is addressed
- Aggressive nail cutting – cutting the nail too short or rounding the corners encourages the nail to grow into the adjacent nail fold and disrupts the cuticle seal in the process
- Cuticle disruption during pedicures – cutting or aggressively pushing back the cuticle removes the barrier between the nail plate and nail fold, leaving the periungual tissue directly exposed
- Prolonged moisture exposure – feet that are frequently wet through sweating, swimming, or occupational exposure become softened and more permeable to microbial entry
- Trauma to the toe – stubbing the toe, dropping an object on it, or repetitive pressure from footwear creates micro-injuries that allow organisms to breach the skin
- Tight or narrow footwear – shoes that compress the sides of the toes against the nail folds can cause sufficient repeated tissue damage to permit infection, particularly during activities that involve extended walking or standing
- Chemotherapy medications – several drug classes used in cancer treatment can disrupt the periungual skin as a direct pharmacological effect, causing paronychia typically 4 to 12 weeks after starting therapy
Who Carries a Higher Baseline Risk?
- People whose feet are frequently wet through work or activity, including healthcare workers, food industry workers, cleaners, and regular swimmers
- People with a history of ingrown toenails, whether current or recurrent
- People with diabetes, where impaired circulation and a reduced immune response mean infections develop more readily and resolve more slowly than in non-diabetic patients
- Patients on chemotherapy or targeted cancer therapies, where the medication directly disrupts the nail fold tissue rather than through immune suppression, often producing multi-nail involvement and periungual pyogenic granulomas
- Immunocompromised individuals, including those receiving immunosuppressants or managing medical conditions that affect immune function
- People who wear narrow, closed-toe footwear for extended periods, particularly in a humid environment where the feet sweat consistently throughout the day
Conditions Commonly Mistaken for Paronychia
Two conditions are regularly confused with paronychia, and the distinction matters because each requires a different approach.
- Ingrown toenail – an ingrown toenail and paronychia frequently coexist, which is part of why they are confused. The distinction lies in the primary problem: in an ingrown toenail, the nail edge itself is pressing into the nail fold and driving the tissue irritation. The redness and swelling in the nail fold are secondary to that mechanical injury. In paronychia, the infection within the periungual tissue is the primary problem. Where both are present at the same time, treating the infection alone without addressing the nail position leads reliably to recurrence.
- Fungal nail infection (onychomycosis) – onychomycosis primarily affects the nail plate itself, causing it to thicken, change colour (typically yellow, white, or brown), and become brittle or crumbly at the edges. The periungual soft tissue is usually not inflamed. Paronychia, by contrast, centres on the nail fold and surrounding tissue rather than the nail plate. The overlap occurs in chronic paronychia caused by Candida, which can affect both the nail fold and the nail plate simultaneously. Clinical examination can distinguish between these presentations, as the treatment approach for each differs meaningfully.

Managing and Preventing Paronychia
Most early-stage acute paronychia responds to conservative care when it is started promptly. The goal at this stage is to settle the infection, allow any accumulated fluid to drain naturally where possible, and prevent the bacteria or fungi from progressing deeper into the tissue. Chronic paronychia requires a longer approach that addresses both the ongoing infection and the conditions keeping the barrier broken.
At the earliest signs of infection, before pus has formed and the inflammation is still confined to the surface tissue, the following measures can contain the problem:
- Warm water soaks for 15 to 20 minutes, three to four times daily, to soften the skin surface and encourage any superficial fluid to drain naturally
- Applying an antiseptic or prescribed topical antibiotic to the nail fold after each soak, once the area has been patted thoroughly dry
- Avoiding further manipulation of the cuticle, nail fold, or nail edge during the acute phase
- Wearing properly fitted footwear that does not press directly against the affected toe, and switching to open-toed footwear at home where practical
Where the infection is bacterial and has progressed beyond the earliest stage, or where visible pus is present under the skin, a podiatrist may need to drain the abscess. This is a straightforward in-clinic procedure that is performed immediately. If the infection has a significant fungal component, targeted antifungal agents should be used in place of or alongside antibiotics. Completing any prescribed antimicrobial course in full matters because partial treatment is a common reason infections return.
For ongoing care and prevention, the focus shifts to protecting the periungual barrier over the longer term:
- Trimming nails straight across rather than rounding the corners, and avoiding cutting them shorter than the tip of the toe
- Keeping the feet dry between activities, using moisture-wicking socks, and allowing the feet to air when at home
- Applying a nourishing cream to the skin around the nail fold to maintain the cuticle without removing it
- Wearing footwear that fits without compressing the toes, particularly during extended periods of standing or walking
- Addressing any biomechanical factors, such as flat feet that load certain toes repeatedly, which contribute to tissue stress at the nail fold.
Management is different from conventional paronychia. Simply stopping the anti-cancer drug is typically not an appropriate option, so treatment is aimed at controlling paronychia symptoms and preventing worsening infection while the patient continues their cancer therapy. This means that a regular visit to a podiatrist every few weeks to months will be necessary, and should be recommended by your oncologist.
Paronychia that keeps returning in the same toe, despite appropriate treatment, usually has an underlying structural driver that has not yet been resolved. The most common is an involuted or ingrowing toenail that has not been addressed at the nail level. A partial nail avulsion removes the nail edge responsible for pressing into the nail fold, which resolves the mechanical trigger for recurrent infection and reduces the likelihood of the paronychia returning.
Have Your Paronychia Managed at Straits Podiatry
Paronychia is easy to underestimate because it often starts with discomfort that seems manageable, and warm water soaks do provide temporary relief. The challenge is that an infection in the nail fold has limited space to resolve on its own, particularly once the skin surface has closed over a pus pocket or when an ingrown toenail is adding repeated pressure to already-inflamed tissue. At Straits Podiatry, assessment focuses on identifying the most likely organism driving the infection, the extent of tissue involvement, whether any abscess has formed, and whether a structural nail issue is contributing to why the infection developed or why it keeps recurring.
From that assessment, a management plan is built around the specific presentation. For straightforward acute paronychia, it typically involves wound care guidance, drainage where an abscess is present, and targeted antimicrobial support. For chronic or recurrent cases, the plan extends to the nail position, nail-cutting technique, footwear fit, and any contributing factors that are specific to the patient. Speak with our team or book a consultation for an assessment and a tailored approach to manage your paronychia.
Frequently Asked Questions About Paronychia
How do I know if my paronychia is bacterial or fungal?
Bacterial paronychia tends to appear quickly, often within hours to a day or two, with visible redness, swelling, warmth, and sometimes pus near the nail margin. The pain is typically sharp and clearly localised. Fungal paronychia, most often caused by Candida, develops more gradually over weeks, tends to produce loss of the cuticle over time, and may cause nail plate changes alongside the periungual inflammation. In practice, the two can be difficult to distinguish without a clinical examination, particularly because chronic presentations may involve a mixed bacterial and fungal component. Treatment differs significantly depending on the cause, which is why a professional assessment is useful before beginning antimicrobial treatment independently.
Can paronychia resolve without treatment?
Very mild acute paronychia caught at the earliest stage, before any pus has formed, may settle with consistent warm water soaks and careful nail hygiene over several days. Once pus has collected beneath the skin, the infection is unlikely to clear without drainage or antimicrobial support, and it may spread or shift to a chronic pattern if left unattended. Chronic paronychia that has been present for weeks or months almost never resolves on its own, because the cuticle barrier has already broken down and the conditions driving repeated infection remain in place.
Is paronychia always linked to an ingrown toenail?
Not always, but ingrown toenails are among the more common triggers for paronychia on the foot. An ingrown toenail creates a persistent wound where the nail edge presses into the nail fold, giving bacteria a reliable route into the periungual tissue. Paronychia can also develop from trauma, prolonged moisture exposure, pedicure-related cuticle disruption, or tight footwear without any ingrown nail being present. Where an ingrown toenail is identified alongside paronychia, addressing the nail edge directly is an important part of resolving the infection rather than managing the periungual tissue in isolation.
How long does paronychia take to heal?
Acute bacterial paronychia treated promptly with the appropriate antibiotic, or with drainage when an abscess has formed, generally settles within one week. Chronic paronychia takes longer because the underlying cause must be managed, not just the infection itself. Where the contributing factors, such as moisture exposure, nail position, and footwear fit, are addressed consistently, meaningful improvement is typically seen within two to four weeks. Full resolution may take longer in cases where the nail plate has already been affected by the chronic inflammation.
When does paronychia need a podiatrist rather than a GP?
A GP can help to manage straightforward acute paronychia with antibiotics or basic wound care. A podiatrist becomes particularly valuable when the infection is recurrent, when an ingrown toenail appears to be driving repeat episodes, when an abscess in the toe needs drainage, or when the nail plate has been affected and the underlying nail structure needs assessment. A podiatrist can examine the nail fold, nail edge, nail plate, and any biomechanical factors contributing to the presentation together in a single consultation, and can address both the infection and its structural cause where one is present.
把这个分享给你认识的人